Capsule Formation around Silicone Breast Implants
Within days of surgery a capsule begins to form around a silicone breast implant. This is the body’s normal response to wound healing around a foreign object that it is not going to reject. The capsule contains scar tissue but it is a little different to a conventional scar on the skin surface. It has minute blood vessels called capillaries and some different types of collagen. There are some white blood cells from the tissue compartment, called T-cells, and some scavenger cells called macrophages. This layer of tissue becomes quite strong but usually remains as thin as tissue paper. It usually remains quite soft and can be quite similar to the lining layer inside your mouth. In 1-2 % of patients per year capsules thicken and tighten and this is called capsular contraction. Bacteria on the implant may increase this problem. Pregnancy and breast feeding may also be associated. The type of implant and its location under or over the muscle may make a difference, with smooth implants placed above the muscle being more commonly affected.
What if my Breast Implant Ruptures?
The capsule is almost always initially protective when a silicone breast implant ruptures because the silicone gel in a good quality implant should be cohesive enough (the silicone molecules all stick together) that the silicone stays put, and the capsule tissue is usually strong enough that it initially does not tear. Modern high quality silicone implants have silicone molecules of a fairly specific size, which are big enough that the molecules do not easily pass through either the shell of the implant or readily through the capsule tissue. Some poor quality implants have too many low molecular silicones in them, and these are small enough to pass through even an intact shell (silicone bleed) and will possibly disperse more readily from a ruptured implant through your tissue capsule. In general, as time passes even with a good quality implant that has ruptured, more of the implant shell will tear until a large rent means the silicone mass is contracting the surrounding capsule. Although silicone is regarded as largely inert, there is some low grade reaction with the capsule in a number of cases. This seems to be a low level of chronic inflammation. The white blood cells in the capsule become more activated and signal for help. This may produce low levels of inflammation with tissue fluid forming, it may signal for the capsule to thicken and begin to change the cells in the capsule. This will not always produce symptoms but it may do so. If the capsule were to tear as well, silicone could pass in the breast lymphatics into the breast tissue where it will form deposits called silicone granulomas, or into the armpit lymph nodes (axilla) forming an enlarged lymph node or group of nodes (silicone lymphadenopathy). It could pass further given enough time. The process is over months rather than days. Detecting at this later stage is far from ideal, but is still treatable. However, once silicone has passed into the tissue it is not usually possible to remove it all. A permanent change is left. Surgery becomes more challenging too.
Some patients capsule tissue reacts more strongly to a rupture and will encapsulate around the implant, with the capsule thickening and contracting. This will manifest as a hard implant. With time it can become rock hard with the implant feeling like a cricket ball. The capsule can also become very fibrous with chalk like deposits inside it. The breast in severe capsular contraction looks distorted and is often painful or aches (grade 4 capsular contraction). A very thick capsule contraction around a ruptured implant is probably less likely to tear and the silicone remains contained inside (intra-capsular rupture). I have seen and dealt with a lot of these cases with patients usually 20-30 years out from their original augmentation having never apparently been advised to consider to have their implant renewal after 10-years. After full capsulectomy and implant renewal the breasts become soft and feel much better again. There is always drop to the breasts because the old capsules also rigidly held the surrounding breast tissue and now the tissue is softer it regains its compliance and stretches.
BIA-ALCL ‘Breast Implant Associated Anaplastic Large Cell Lymphoma’
A lympho-proliferation can occur of the T-cells (the tissue white blood cells) if they are constantly stimulated. Researchers are studying this as the exact cause is uncertain. The cancerous change is called breast implant associated anaplastic large cell lymphoma and it is a progression that is of cause a huge concern. It is rare over a woman’s lifetime with breast implants but seems definitely more common with the macro textured surface implants. One year ago, an Australia study put the risk at around 1 in 35oo women over a 10-year period with their macro-textured implants. This is therefore extremely unlikely to occur but given the risk is around 1 in 60,000 women over a 10-year period with micro textured silicone implants, there are clues as to what contributes. And many surgeons like me are now using microtextured or no texture when we place implants. The risk with smooth shelled implants if you have never had a textured implant is currently (as of January 2018) thought to be negligible.
BIA-ALCL appears usually with the sudden appearance of a fluid collection between the implant and capsule- an effusion (or sometimes called a seroma), or it can present more advanced with a mass. Untreated BIA-ALCL can become a killer, so any woman with changes should see a specialist with experience or good knowledge of the disorder so that checks can be made. If there is a suspicion, tests can usually be done pre surgery. But if you are having implant exchange and you have a change in the capsule or fluid around the implant, ensure your surgeon is going to consider full capsulectomy.
Complete Capsulectomy at the time of Breast Implant Removal or Exchange
Capsulectomy can be time consuming and some surgeons may not like doing it. It adds to the cost of your surgery too. Some surgeons may not be quite as good at doing a capsulectomy as others who do these operations more commonly. If during the dissection the surgeon penetrates the capsule it can be harder to remove it all, particularly if the implant is ruptured as sometimes silicone comes out of the hole and interferes with the operation. However, if you are under a specialist who has done hundreds of capsulectomies, with patience you can achieve a 100% capsulectomy in most cases without significant disruption. The entire implant is removed still contained within it’s capsule. Once out and the surgeon has finished the operation he or she can dissect the capsule off the implant to inspect the insider layer looking for any clues as to a problem. The implant is inspected too to see if it was intact or ruptured. The capsule can be sent for routine histo-pathology, where if there are any concerns under a microscope, the pathologist can order special tests called immuno-histochemistry looking at the tissue with special antibodies attached to a coloured dye to reveal the cell types the pathologist is concerned about that might signal abnormal disease. For example in BIA-ALCL where cancerous T-Cells are forming that are a type of lymphoma, the test is called CD30, and if positive over a significant local area of capsule it signals the presence of the lymphoma.
If you were to have had a BIA-ALCL which is in the early stages confined to the capsule, the capsulectomy is regarded as likely curative treatment. If your capsulectomy was not complete it is a concern and surgery might be required again. You may need chemotherapy or other treatment too. The surgeon’s note keeping is very important here, as if they have recorded it as a capsulectomy but it was not 100%, they will have left bits of capsule in some recesses, and if that happens to be where the BIA-ALCL was, recurrence will likely follow.
Capsulectomy for Capsular Contraction
A capsular contraction normally distorts the breast once advanced and my preference is a full capsulectomy to get back to soft tissue. I still send the capsule tissue to histology though it is very likely to be non cancerous in every case- as has been the situation in my doing this for the last 14 years!
Very occasionally it might be necessary to leave capsule or do a capsulotomy instead and the surgeon would document this and the reasons. This might be because the capsule tissue is so adherent to rib or inter-costal muscle that the risk of bleeding or harm is too great and disproportionate to the problem being dealt with. If the remaining breast tissue is very thin and capsule looks normal in places it might be preferable to leave some. An experienced surgeon makes these judgements in your best interests.
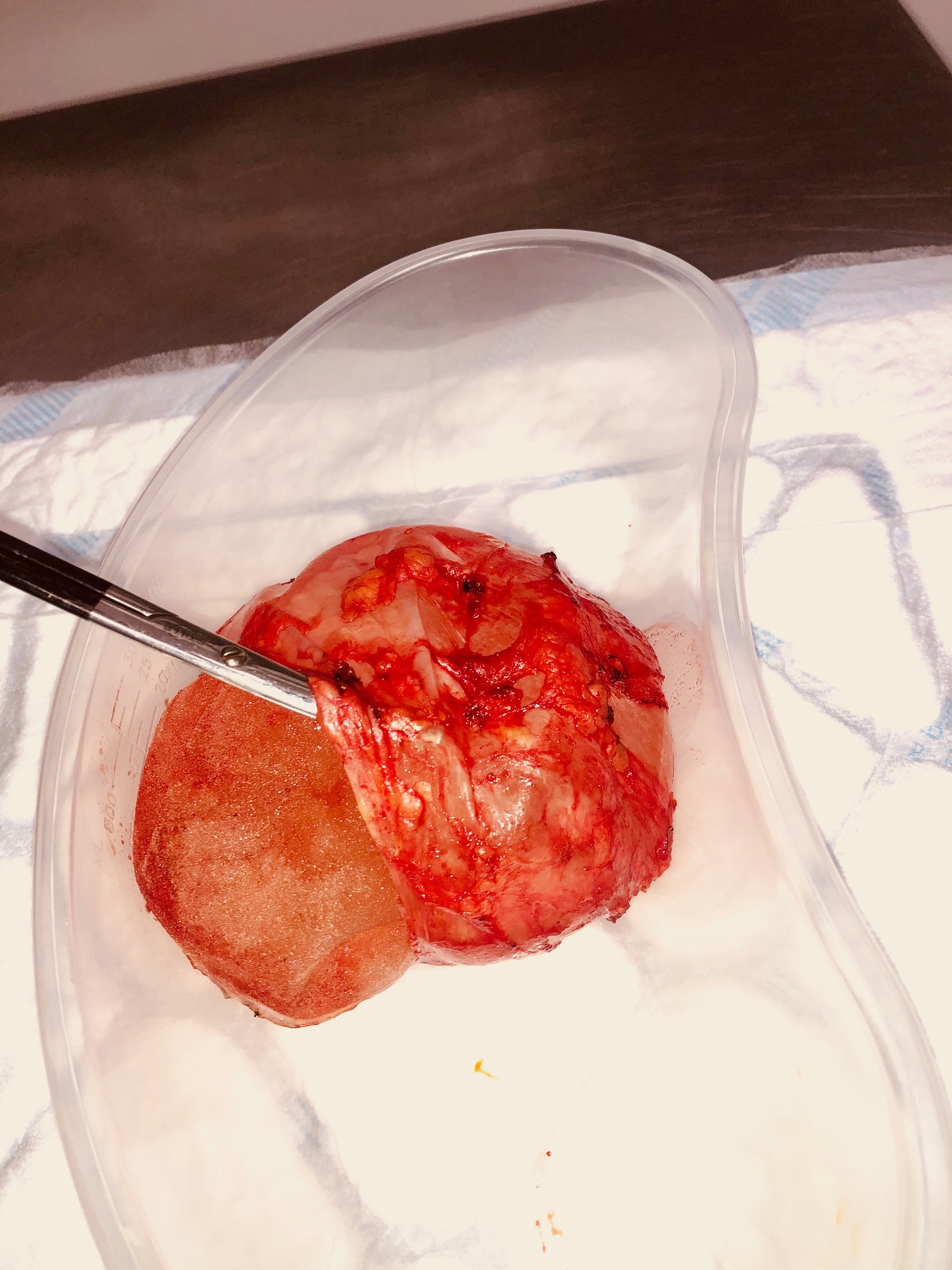
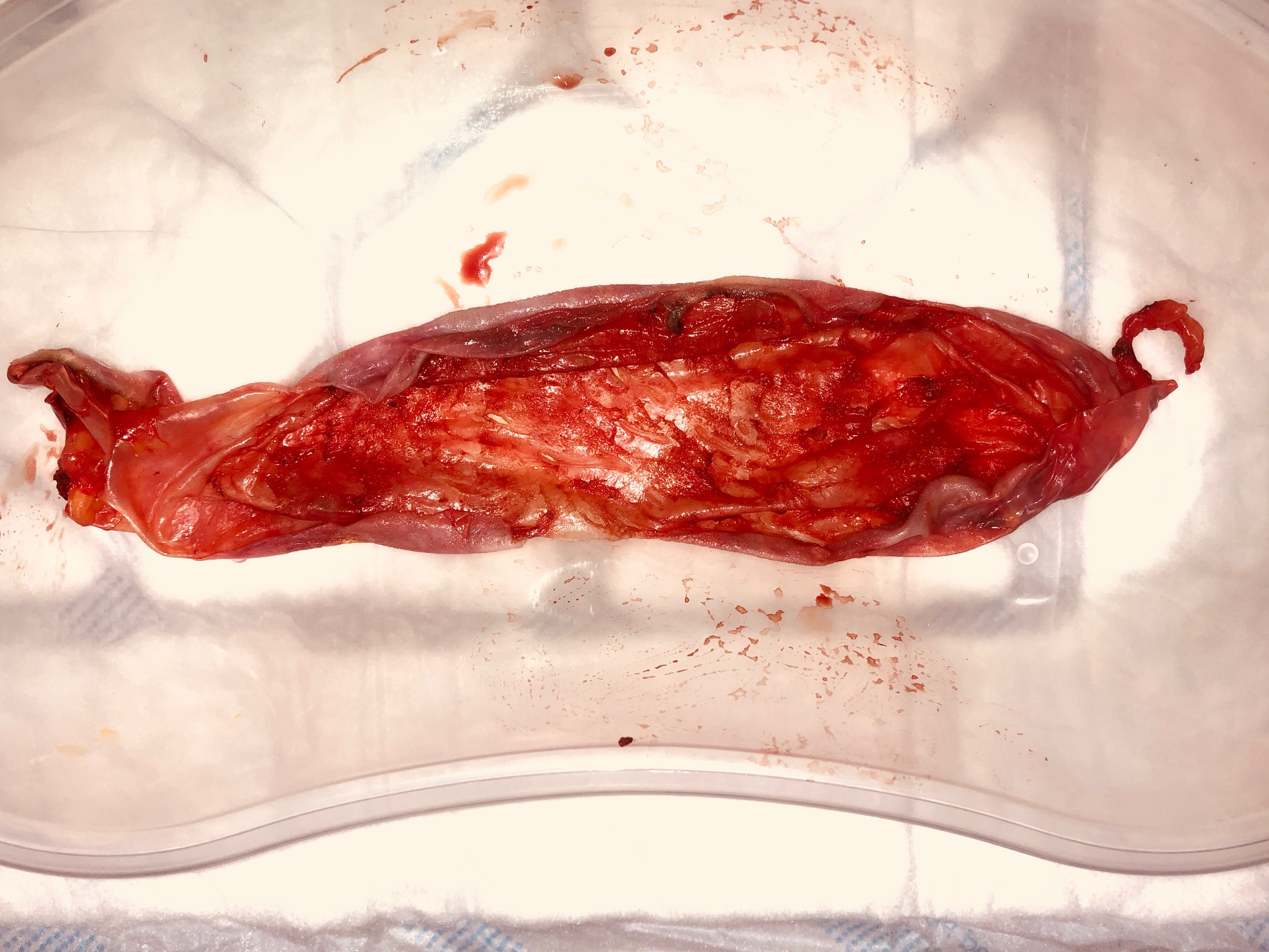
The photos I have included here were for a simple case of capsular contraction around a silicone breast implant that was not ruptured. I performed capsulectomy and removed the old implants. At this stage we have left the implants out. The capsule tissue has been sent for routine histopathology.